
This article discusses the diagnosis, treatment, complications, and lifestyle factors that can increase your risk of developing pregestational diabetes. This condition is particularly common in Saudi Arabia, which has an estimated prevalence of 36%. Moreover, the prevalence of T2DM in the population is high, and the epidemiology of GDM is closely related to that of T2DM.
Table of Contents
Treatment of pregestational diabetes

Treatment of pregestational diabetes is very important for preventing complications and maximizing the chances of a healthy pregnancy and delivery. It requires multidisciplinary approaches and a comprehensive approach to reduce maternal and fetal morbidity. The aim of treatment is to keep blood glucose levels close to normoglycemia, which is the lowest level possible. Good glycemic control during pregnancy helps to reduce the risks of adverse pregnancy and delivery outcomes, including preeclampsia, macrosomia, and congenital malformations.
Medical nutrition therapy is also an important part of pregestational diabetes treatment. The recommended daily diet for women with pregestational diabetes is 175 g carbohydrate, 71 g protein, and 28 g fiber. It is also important to monitor blood pressure, which typically drops during the second trimester. The target blood pressure level should be around 130/85 mmHg.
If you have pre-existing diabetes and are concerned about your health, visit your provider. Discuss your diabetes treatment plan with your provider, and let them know that you're pregnant. The two of you will work together to get your pregnancy ready and stay healthy during the pregnancy. They will also make sure that the treatment you're receiving is safe for you and your baby.
Treatment of pregestational diabetes requires close monitoring throughout the pregnancy and postpartum period. During the pregnancy, a woman with pregestational diabetes may need to change her medication and insulin dosage. In addition, many medications used to treat diabetes should be stopped before conception. This is especially important for those who take thiazolidinedione medications.
If you are planning a pregnancy, consider a low-dose aspirin to prevent preeclampsia. This medication, also known as baby aspirin, is safe and has been shown to decrease the risk of preeclampsia. This drug can be started after 12 weeks of pregnancy and should be stopped before 16 weeks of pregnancy.
Diagnosis
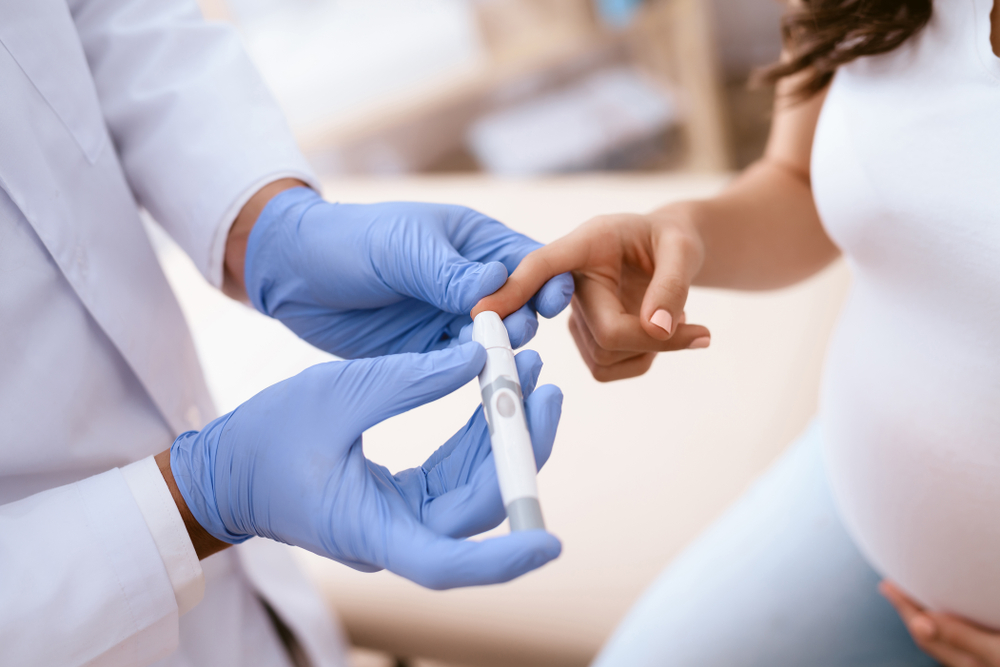
In the United States, approximately 1% to 2% of pregnant women have pregestational diabetes. The prevalence of diabetes in this group is increasing because of sedentary lifestyles and poor diets. Despite its increasing prevalence, pregestational diabetes is not common. Pregnant women who have diabetes should speak to their health care providers to get a proper diagnosis.
The first step in a pregnancies diabetes diagnosis is to determine the gestational age of the pregnant woman. Depending on gestational age, the diagnosis of pregestational diabetes may be delayed or not possible. The use of MPHRR enables the coupling of diabetes in pregnancy and childbirth.
Diagnosis of pregestational disease is essential to reducing the risk of complications for the baby and mother. Insulin is the standard pharmacological treatment for women with pregestational diabetes. However, more research is needed to determine if metformin is a good option in this context.
Administrative health data are a valuable resource for longitudinal studies in health care. They are comprehensive and population-based. Because the effects of pregestational diabetes can be passed on to the child, validation of the case definition is important. This study used administrative data to compare the definition of pregestational diabetes among 199 mother-child dyads.
Pregnant women with known impaired glucose metabolism should be screened for GDM. Screening should begin as early as 24 weeks of gestation. The goal is to reduce the immediate health consequences of the condition and minimize the potential for long-term complications. The recommended screening method is a two-hour OGTT followed by a glucose challenge.
Treatment

Diabetes during pregnancy, also known as pregestational diabetes, must be managed carefully to avoid complications for the mother and fetus. The goal of pregestational diabetes management is to keep blood glucose levels near normoglycemic levels. This level is lower than that in women who do not have diabetes, and it reduces the risk of adverse maternal and fetal outcomes, such as preeclampsia and macrosomia.
A proper treatment plan for gestational diabetes includes regular blood glucose testing, physical activity, and special diet plans. Insulin may also be used to control blood glucose levels. The American Diabetes Association recommends that women who have gestational diabetes follow specific blood glucose targets during the pregnancy. Women with diabetes should monitor their blood glucose levels at least once per day and take insulin as directed by their health care team.
The first step in treating gestational diabetes is to understand what type of diabetes you have. The initial glucose challenge test involves drinking a syrupy glucose solution and receiving a blood test. If your blood glucose level is over 190 mg/dL or 10.6 mmol/L, you have gestational diabetes. In most cases, blood glucose levels below that level are considered normal.
In addition to the risk of gestational diabetes, women with gestational diabetes may also be at higher risk of a fetus developing ALL. In the past, the association between gestational diabetes and childhood ALL was unclear, but new research has shown that the conditions can be linked.
During pregnancy, diabetes increases the risk of delivery through c-section, so women with diabetes should get regular blood glucose tests to check if they are at risk for diabetes. Women should also ask their health care providers about the timing of c-section. While some women are able to wait until 39 weeks, others may have to deliver earlier because of complications. The health care provider will also monitor blood glucose levels during labor and delivery, and they can administer insulin if needed.
There are many complications associated with diabetes during pregnancy, including increased risk for infants, increased risk for cesarean delivery, and increased NICU admission. Those risks are far greater in women with diabetes than those without it.
Complications

Pregnant women with diabetes are at higher risk of complications, particularly preterm labor and delivery. Generally, pregestational diabetes results in poorer pregnancy outcomes and affects both the mother and fetus. While the disease itself has no cure, it can be managed during pregnancy, and some strategies for managing pregestational diabetes are different than those for normal gestational diabetes.
The goal of medical management of pregestational diabetes is to maintain maternal blood glucose levels at near or above normoglycemia. Normoglycemia is the lowest level of blood glucose for pregnant women who do not have diabetes. Good glycemic control during pregnancy reduces the risk of maternal and fetal complications, such as preeclampsia, macrosomia, and congenital defects.
Maternal pregestational diabetes mellitus is associated with a significantly increased risk of fetal CHD. The risk was independent of the type of diabetes and the timing of onset. Moreover, the duration of gestational diabetes mellitus did not influence the risk of fetal CHD.
Uncontrolled diabetes during pregnancy can result in an extra-large baby or a premature delivery. It can also cause shoulder dystocia during vaginal delivery. In this case, the shoulders of the baby can become trapped behind the pubic bone. These problems can increase the risks of birth trauma. Pregnant women with gestational diabetes can also develop preeclampsia, which can lead to premature delivery or even stillbirth.
A woman with pre-existing diabetes is at risk of major malformations during pregnancy if her A1c level is above 260 mg/dl before conception. A recent study of 1,676 women with pre-existing diabetes found a high rate of anomalies during pregnancy. While women with A1c levels of 10% or higher had a high risk of anomalies, women with A1c levels of 13% or higher had a much lower risk.










